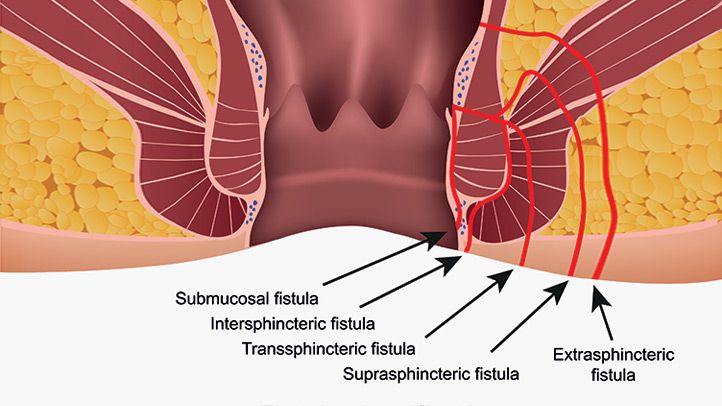
What is an Anal Fistula?
An anal fistula is a tunnel connecting an infected cyst in the anus to an opening on the skin surrounding the anus. When small glands that produce mucous inside the anus get clogged and infected, it forms abscess or cyst, explains Dr. Purnendu Bhowmik, the best fistula surgeon in Kolkata. Half of these abscesses have a chance of developing into a fistula.
What Causes Fistula in Ano?
The leading cause of an anal fistula is clogged anal glands that produce mucous and anal abscesses. Other rare conditions that can lead to the development of anal fistula are:
- Crohn’s disease
- Radiation Therapy
- Injury to the anal canal
- Sexually transmitted diseases
- Tuberculosis
- Diverticulitis (a disease that leads to the formation of small pouches in the large intestine that become inflamed)
- Cancer
 Call Now:
8010 552 552
7595 838 844
Call Now:
8010 552 552
7595 838 844
 Whatsapp Now:
8010 552 552
Whatsapp Now:
8010 552 552
 Email Me:
[email protected]
Email Me:
[email protected]